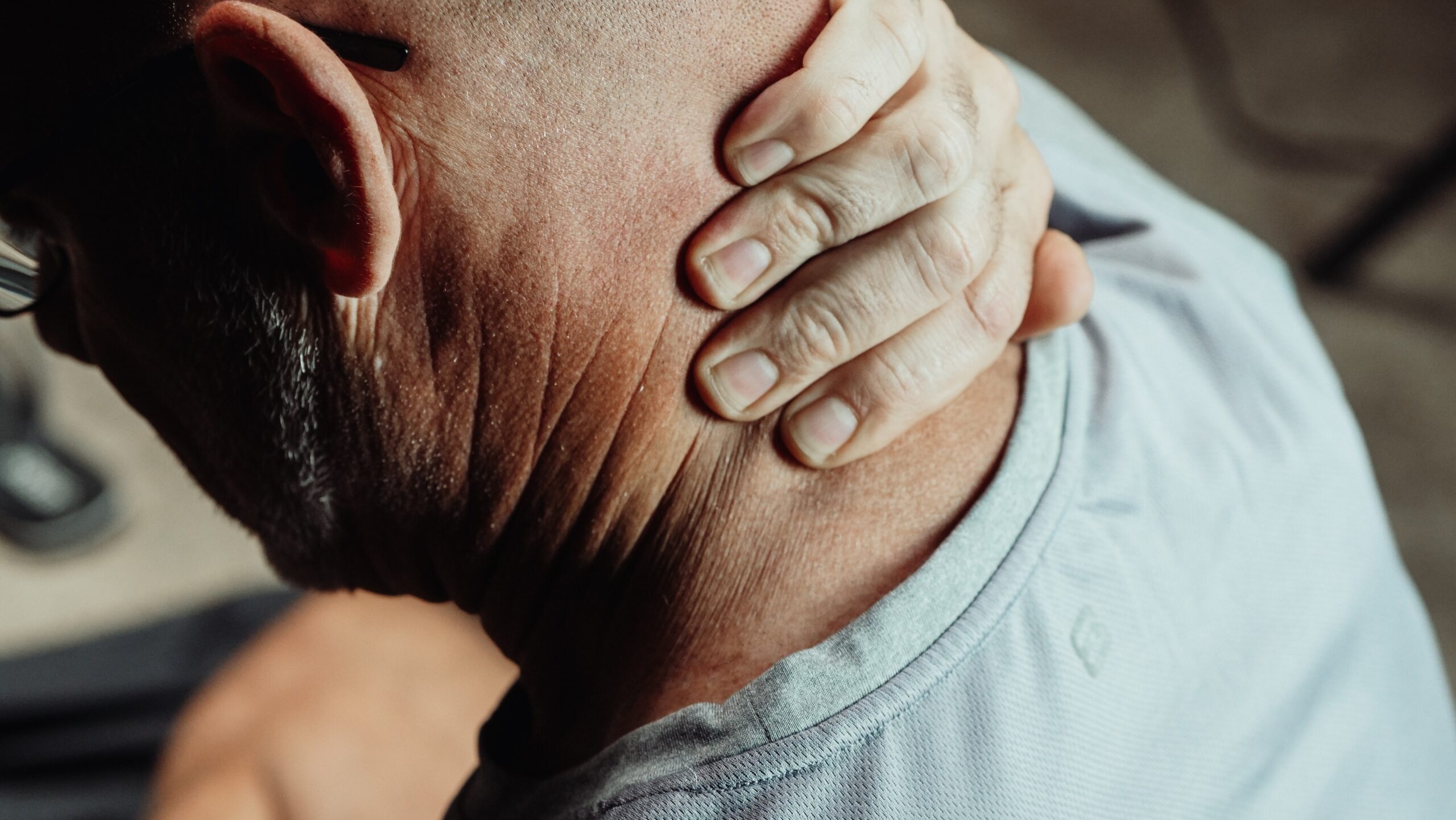
Fibromyalgia is a chronic condition resulting in pain all over the body which can be accompanied by numerous symptoms including mood changes, cognitive difficulties and fatigue. Although research indicates fibromyalgia to be more prevalent in women, men are affected too.1 This may leave you thinking, what are the symptoms of fibromyalgia in men?
In this article, learn about fibromyalgia symptoms in men and take the fibromyalgia self-test to go through the symptom checklist.
Why Fewer Men Are Diagnosed with Fibromyalgia
Can men have fibromyalgia symptoms? Most definitely! Men can experience the same symptoms of fibromyalgia as women do. However, fewer men may be diagnosed. One research study found that although men might meet fibromyalgia survey criteria in research, they are less likely to be given a diagnosis of fibromyalgia2
So, what is the reason for a lower diagnosis rate of fibromyalgia in men? The short answer is we don’t know for certain, but a few theories have been suggested:
- Some doctors have hypothesized that lower rates of fibromyalgia in men could be due to the way society expects men and women to respond to pain. Men are viewed or may view themselves as someone who should not feel or disclose pain.
- Also, hormonal changes women experience through menstruation and menopause are also linked with fibromyalgia, resulting in a higher diagnosis rate in females.
- Some research has indicated that men are also less likely to visit healthcare providers, meaning that since they are not seen for what could be fibromyalgia pain, no diagnosis can be made.2
- Tender point theory could also be another factor. Tender points, which were used in the past to diagnose fibromyalgia are specific tender areas in the body that when pressed or touched can result in widespread pain.3 Women have been shown to have more tender points than men,4 which is also why this exam is no longer recommended as part of a fibromyalgia diagnosis.
Let’s take a look at a couple of these in more detail.
Gender Stereotypes in Chronic Pain
As mentioned, many chronic pain conditions like fibromyalgia can come with gender stereotypes. Men may view themselves, or society might view them as people who should not disclose much pain. On the flip side, women may not see themselves, or may not be viewed by others, in this way.
These stereotypes about experiencing pain can lead to men being less likely to come forward to anyone about their pain.2 It’s not uncommon for men to hold the belief that they should not go to the doctor about pain, or they’re not supposed to complain. This may result in fewer men being diagnosed with fibromyalgia. Unfortunately, this can result in more difficulties later in life if the pain is not addressed or believed.
In summary, men may have difficulties with fibromyalgia symptoms just as frequently as females; however, they may be less likely to come forward due to these gender stereotypes, resulting in a gender bias.
Tender Point Theory
Another reason why fewer men may be diagnosed with fibro is due to biases in the tender point theory. Tender points are areas of tenderness around joints that can hurt and result in pain around the body when pressed. These used to be used as part of the diagnostic criteria for fibromyalgia.
However, research indicates that females with fibromyalgia have more tender points and experience more pain at these tender points than men do.5 Therefore, if women have more of these tender points, they may be more likely to feel pain around the body compared to men, which characterizes fibromyalgia. This bias contributed to tender point exams no longer being used in fibromyalgia diagnosis, according to the 2016 American College of Rheumatology guidelines.
Again, gender stereotypes in chronic pain may feed into this. Men may report less pain in these tender points so that they are not seen as experiencing a lot of pain. Therefore, the tender point theory is unlikely to contribute alone to fewer men being diagnosed with fibromyalgia. Instead, it could be a combination of other factors such as gender stereotypes and/or hormonal changes in females throughout life compared to males which can impact pain experienced.
Fibromyalgia Symptom Checklist
Although fewer men are diagnosed with fibromyalgia (which can be due to multiple factors), men can and do experience fibro symptoms. Let’s take a look at the symptoms of fibromyalgia in men.
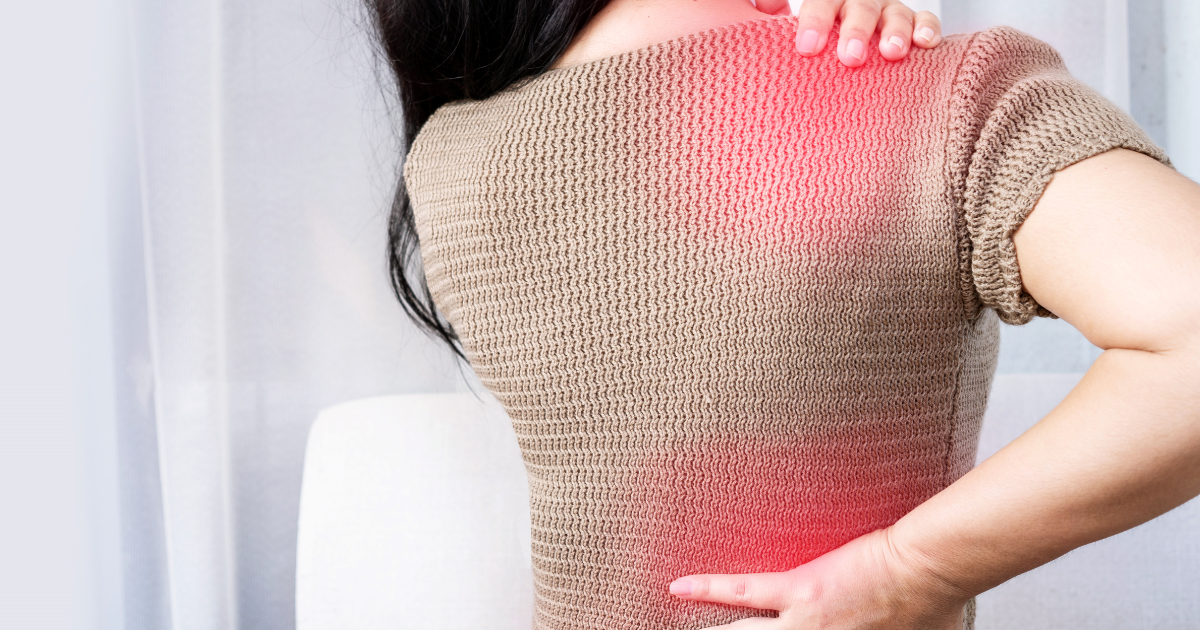
Chronic Whole-Body Pain
The hallmark symptom of fibromyalgia is chronic whole-body pain, in both males and females. The underlying mechanism for this is thought to be due to a process called central sensitization; long-lasting and more severe pain can be the result of the way in which pain is processed in the central nervous system (CNS).6
Brain imaging studies7 provide evidence for the role of central sensitization in chronic whole-body pain. These studies have found increased connectivity in systems that amplify pain signals, and reduced connectivity in systems that reduce the processing of pain.
Pain experienced for longer than three months is characterized as chronic, and for pain to be ‘whole body,’ it must be felt in at least four out of five areas:
- Right upper region (shoulder, arm)
- Left upper region (shoulder, arm)
- Axial region (neck, back)
- Left lower region (left hip, leg)
- Right lower region (right hip, leg)
Although women with fibromyalgia may have a higher perception of whole-body pain than men with fibro8, a recent 2023 review of the research found men to have more painful experiences and more catastrophic thoughts about whole-body pain.9 However, due to the lower diagnosis rate of fibromyalgia in men, these studies reviewed had a small sample size, limiting the conclusiveness of these results.
Fatigue and Sleeplessness
Fatigue and sleeplessness are also common symptoms of fibromyalgia in men. One study found out of 805 men with fibromyalgia, 75% of them reported experiencing fatigue and sleeplessness.10
Sleep difficulties have been found to occur frequently in individuals with fibromyalgia; sleep difficulties can range between having reduced sleep quality, duration, and efficiency, as well as increased sleep disturbance.11
A recent qualitative study helped conceptualize the experience of fatigue and sleeplessness in men in more detail.12 The men described fatigue as continuous and always present; not subsiding even with rest; and having serious impacts on their lives including limiting activity, making ‘conditioned’ jobs harder (for example, peeling potatoes and having to give themselves a break due to the fatigue) and having difficulties holding things due to how tired they are.
In the same study, men also described non-physical impacts of sleep disturbance, such as waking up frequently in the middle of the night, not being able to go to sleep due to worrying thoughts, and these sleep difficulties affecting their mood.12
As you can see, fatigue and sleeplessness can affect men with fibromyalgia in different ways. If you are having difficulties with sleep and fatigue, it is important to speak to your doctor to see what can help.
Cognitive Symptoms
Cognitive symptoms, which are also termed brain fog or “fibro fog,” include a variety of symptoms such as:
- Finding it difficult to think straight
- Problems with attention and concentration
- Inhibited verbal skills such as slow speech
- Forgetting things
Evidence for fibro fog has come from a variety of studies; one review of 37 studies compared individuals with fibromyalgia with people without fibromyalgia on a variety of neuropsychological measures.13 Cognitive difficulties such as difficulties with processing speed and memory were consistently found in individuals with fibro.
Specifically within men with fibromyalgia, research has found cognitive difficulties to range from very mild concentration difficulties to severe difficulties with problem-solving and memory.14 This study also examined the impact these symptoms had on men, including difficulties with work and relationships, and impact on mood and anxiety.
If you are experiencing any cognitive symptoms, discuss this with your doctor to see what can help.

Take the Fibromyalgia Self-Assessment
The fibromyalgia symptoms list in men is the same as the symptoms women report. However, just like with pain, the experience of these symptoms can differ in men and women.
Because of the variety of symptoms, it can be helpful to take your own fibromyalgia self-assessment. You can take the fibromyalgia quiz here to go through the diagnostic criteria on your own and get your score to discuss with a doctor.
Medically reviewed by Dr. Andrea Chadwick, MD, MSc, FASA
Sources
- Ruschak I, Montesó-Curto P, Rosselló L, Aguilar Martín C, Sánchez-Montesó L, Toussaint L. Fibromyalgia syndrome pain in men and women: A scoping review. Healthcare (Basel). 2023 Jan 11;11(2):223. doi: 10.3390/healthcare11020223. PMID: 36673591; PMCID: PMC9859454.
- Vincent A, Lahr BD, Wolfe F, Clauw DJ, Whipple MO, Oh TH, Barton DL, Sauver JS. Prevalence of fibromyalgia: A population based study in olmsted county, minnesota, utilizing the rochester epidemiology project. Arthritis Care & Res. 2012 Nov; 65(5): 786-792.
- Jahan F, Nanji K, Qidwai W, Qasim R. Fibromyalgia syndrome: an overview of pathophysiology, diagnosis and management. Oman Med J. 2012 May;27(3):192-5. doi: 10.5001/omj.2012.44. PMID: 22811766; PMCID: PMC3394355.
- Wolfe F, Cathey MA. The epidemiology of tender points: a prospective study of 1520 patients. J Rheumatol. 1985 Dec;12(6):1164-8. PMID: 3879278.
- Arout CA, Sofuoglu M, Bastian LA, Rosenheck RA. Gender Differences in the Prevalence of Fibromyalgia and in Concomitant Medical and Psychiatric Disorders: A National Veterans Health Administration Study. J Womens Health (Larchmt). 2018 Aug;27(8):1035-1044. doi: 10.1089/jwh.2017.6622. Epub 2018 Apr 2. PMID: 29608126; PMCID: PMC6425926.
- Nijs J, George SZ, Clauw DJ, Fernandez-De-Las-Penas C, Kosek E, Ickmans K, Fernandez-Carnero J, Polli A, Kapreli E, Huysmans E, Cuesta-Vargas AI, Mani R, Lundberg M, Leysen L, Rice D, Sterling M, Curatolo M. Central sensitization in chronic pain conditions: Latest discoveries and their potential for precision medicine. Lancet Rheumatol. 2021 May;3(5):E383-E392. doi:10.1016/S2665-9913(21)00032-1
- Cagnie B, Coppieters I, Denecker S, Six J, Danneels L, Meeus M. Central sensitization in fibromyalgia? A systematic review on structural and functional brain MRI. Semin Arthritis Rheum. 2014 Aug;44(1):68-75. doi: 10.1016/j.semarthrit.2014.01.001. Epub 2014 Jan 8. PMID: 24508406.
- Yunus MB. The role of gender in fibromyalgia syndrome. Curr Rheumatol Rep. 2001 Apr;3(2):128-34. doi: 10.1007/s11926-001-0008-3. PMID: 11286669.
- Ruschak I, Montesó-Curto P, Rosselló L, Aguilar Martín C, Sánchez-Montesó L, Toussaint L. Fibromyalgia Syndrome Pain in Men and Women: A Scoping Review. Healthcare (Basel). 2023 Jan 11;11(2):223. doi: 10.3390/healthcare11020223. PMID: 36673591; PMCID: PMC9859454.
- Muraleetharan D, Fadich A, Stephenson C, Garney W. Understanding the Impact of Fibromyalgia on Men: Findings From a Nationwide Survey. Am J Mens Health. 2018 Jul;12(4):952-960. doi: 10.1177/1557988317753242. Epub 2018 Feb 1. PMID: 29388465; PMCID: PMC6131475.
- Keskindag B, Karaaziz M. The association between pain and sleep in fibromyalgia. Saudi Med J. 2017 May;38(5):465-475. doi: 10.15537/smj.2017.5.17864. PMID: 28439595; PMCID: PMC5447206.
- Ruschak I, Toussaint L, Rosselló L, Aguilar Martín C, Fernández-Sáez J, Montesó-Curto P. Symptomatology of Fibromyalgia Syndrome in Men: A Mixed-Method Pilot Study. Int J Environ Res Public Health. 2022 Feb 2;19(3):1724. doi: 10.3390/ijerph19031724. PMID: 35162747; PMCID: PMC8834813.
- Bell T, Trost Z, Buelow MT, Clay O, Younger J, Moore D, Crowe M. Meta-analysis of cognitive performance in fibromyalgia. J Clin Exp Neuropsychol. 2018 Sep;40(7):698-714. doi: 10.1080/13803395.2017.1422699. Epub 2018 Feb 1. PMID: 29388512; PMCID: PMC6151134.
- Sallinen M, Marit Mengshoel A. Memory gaps, lost words and crucial mistakes – Men’s experiences of cognitive difficulties in fibromyalgia. Chronic Illn. 2021 Mar;17(1):41-52. doi: 10.1177/1742395318815947. Epub 2018 Dec 26. PMID: 30587007.